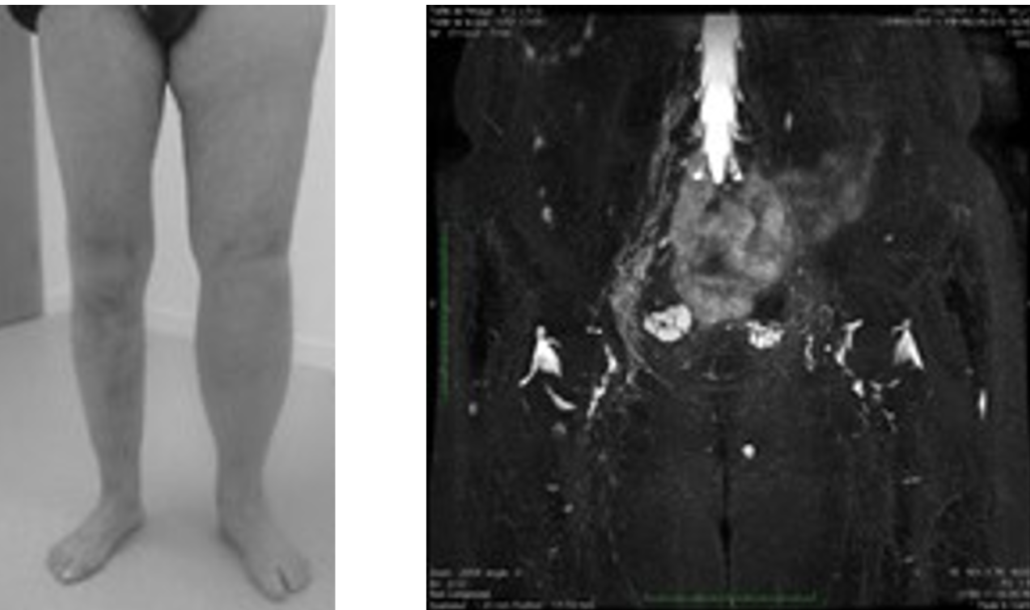
IATROGENIC LEG LYMPHEDEMA
Introduction
Symptomatic lymphoedema is frequently associated to severe morbidity, including pain and feeling of heaviness of the affected limb, disability on the daily activities and serious aesthetic concerns. Moreover, lymphoedema patients are prone to develop recurrent infection episodes, which may present as cellulitis, erysipelas or lymphangitis, requiring oral antibiotic treatment and -quite frequently- long hospitalization for intravenous antibiotic therapy. The psychosocial impact of lymphoedema in breast cancer related lymphoedema (BCRL) patients has been described to be as distressing, as the initial diagnosis of breast cancer.
Management of lymphoedema traditionally consisted of conservative treatments, including manual lymphatic drainage, compression garments, pneumatic pumps and multilayer bandaging. Recently, microsurgical procedures, namely vascularized lymph node transfers, lymphaticovenous anastomoses, lymphatic-venous-lymphatic plasties and lymphaticolymphatic grafts are being used in an increased fashion and considered to offer an effective treatment to severe lymphoedema cases.Actually, the combination of the lymphnode transfers, liposculpture and locally Lymphovenous anastomosis are preferred.
Corinne Becker has pioneered the introduction of vascularized lymph node flap and described the lymph node transfer (LNT) technique as a logical reconstructive approach of the lymphoedema sequelae; the flap bridges the injured and interrupted lymphatic pathways and reestablishes the lymphatic flow by promoting lymphangiogenesis. Saaristo et al, studied the mechanism of lymphagiogenesis following LNT and advocated that the vascularized lymph nodes promote the procedure by activating growth factors, such as VEGF-C. The long-term advantages of this microsurgical approach include permanent limb volume reduction, decreased number of infection episodes and total improvement in the quality of patients’
Secondary lymphedemas are common in oncologic treatment, especially after lymph node dissection and radiotherapy.
Cancers, whose treatments are commonly associated with lymphedema, include pelvic tumors (i.e., enlarged hysterectomies and prostatectomies),Hodgkin’s tumors, sarcoma and melanoma.
Alternatively, lymphedema may also be caused by non-oncologic procedures such as saphenous vein removal, hernia repair, or thigh lifts, internal liposuctions.
The lymphedema can appear immediately or many years after the surgery. Chronic infections can destroy all the remaining lymphatic collectors and elephantiasis can occur with skin thickening, folds , redness, fibrosis.
Diagnosis
The diagnosis is made by clinical examination, and lymph MR (map of the lymphatic situation)
Physical Treatment
Physiotherapy with manual drainages, bandages, compression garments is necessary, but sometimes inefficient.
Best Surgical Treatment
Excisions
Wedge excisions in elephantiasis are sometimes needed to avoid mycosis in the deep folds, and to allow bandaging. Free nodes transplantation are done the same day, or later regarding the extension of the resection
Autologous Lymph Nodes Transfers
The reimplantation of some nodes to reestablish the connections between the remaining nodes and chains can improve the drainage of the limb. Because healthy nodes contain VGEFc, a natural lymphatic growing hormone, they promote the development of new channels. Sometimes 2 flaps are needed to improve the results :one in the inguinal area, one in the knee region, if the lymphoedema is advanced.
Liposculpture
Autologous Lymph Node Transfer can be combined with local liposculptures, with the fluoroscopy to localize the lymphatic vessels,and reduce the possibility to dammage the remaining lymphatic vessels. A selective external liposculpture can remove the « entrapped » fat and improve the aesthetic results.
The fat macromolecules are carried by the lymphatic vessels. In case of hypoplasy, the hyperpression in the very fine superficial lymphatic vessels , open the mini ducts interconnections, and the fatty molecules are going through and will stay for ever under the skin.
Results
For the lower leg, the results are really correlated to the duration of the lymphedema, the fibrosis and, of course, the bilateral defect of the iliac lymphatic chains.
The lymphatic MRI shows new lymphatic pathways normalization of the lymphatic pathways in moderated cases. In long term lymphedema, 1 year after LNT, transformation in lipedema can occur.
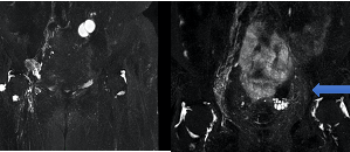
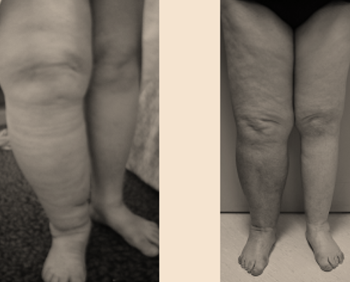
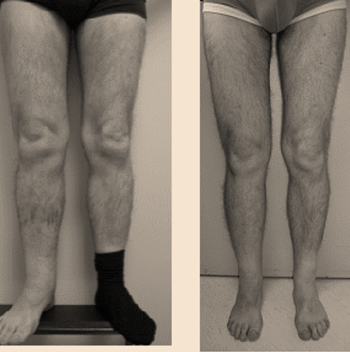
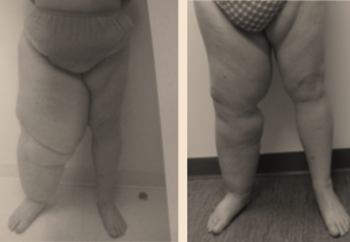
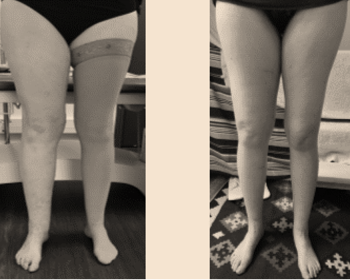
The results are showing a dramatic reduction of the infections, reduction of the volume, mostly after the second transfer if elephantiasis.The lipoosculpture helps to reduce the fat absorption in the lymphoedema limb.Some cases can. be completely healed (moderated) and the elephantiasis can be reduced from 80%..
Complications are infections, hypertrophic scars, hematoma, but never degradation of the situation and no edema of the donor cases (if weel operated !!! needs a lot of experience, difficult donor flap !!!)